Case studies for HEE project on profession specific interventions

Nick Knight
Podiatrist in independent practice
Case study
Nick Knight: podiatrist in independent practice
My research journey
Research has always been something that has interested me within podiatric practice. Working in both the NHS and private sector, I have noted first-hand the challenges involved in conducting and implementing research into clinical practice due to pressures such as appointment numbers, time, and resources.
'It has been exciting going on this journey of blending education, research, and enterprise to try to benefit clinical practice’
So why the interest?
In a nutshell, the use of research evidence supports my ability to provide care to patients that is contemporary and up-to-date with the latest technology and interventions. Through research, there is an opportunity for success, in terms of patient outcomes, which can lead to improved team morale and environment. The common phrase ‘success breeds success’ rings true. Research findings can provide evidence that podiatrists are clinically and cost-effective in delivering patient care. Anecdotal evidence and single clinician/practice claims are no longer listened to when bidding for work as society today demands data and evidence to substantiate those claims. In providing evidence, the research data supports the narrative we are trying to tell and showcases the podiatric interventions or ideas and advice that we know will improve patient lives.
The journey
My journey started when I was doing my MSc. I will be completely honest; I was a numbers guy and I was fixed on quantitative data. However the research module on my MSc opened my eyes to qualitative methods and the importance of being able to show impact through understanding the experiences and opinions of my patients.
Whilst building my clinical caseload in the private sector I was also managing a growing family. Initially, I started to rent rooms from fellow practitioners and started to build a team around me. Consequently, I started to change my thinking and focused on trying to understand whether we deliver what we say we are going to deliver, how can I measure this and how can I be sure we are doing this well? My approach started to evolve, and I wanted to know what questions or patient reported outcome tools should I be using to identify how a patient’s treatment journey went. I also wanted to know about patient satisfaction scores, the length of time the treatment plan takes to complete and how many appointments on average patients need.
As a result, through my practice, I created our clinical templates on the Cliniko system (a patient management programme), Microsoft Forms and CliniqApps using evidenced-informed practice. This allowed us to automatically send questionnaires to patients after the treatment had finished. This continued for around 9-12 months.
At the time, I thought things are going okay and the clinical team were doing well. I then received an email from Dr Charlotte Dando (Charlie) about participating in her PhD study as part of a consensus exercise on Morton’s Neuroma. Charlie was also keen to observe my clinical practice and by the end of the few days I offered her a job. She was a little surprised and thought I was joking!
Charlie and I started to review the clinical data specific to pathology. We realised we could be doing better and a solution to this would be for me to take the next step and have my own premises for the business (Peppermill Barn, Romsey). Although I had established links with surrounding Higher Education Institutes (HEIs), Charlie provided the equilibrium to allow both businesses to work together.
Once settled into the new clinic, we decided that we needed some help and guidance. Professor Cathy Bowen, Dr Lucy Gates, Charlie, and I over a few teas, formulated the clinical questions we wanted to ask. Those questions are still reviewed for relevancy and are still in use today. We now have over 350 completed patient journeys, in addition to the 6, 12 and 18-month follow-up data. It's lovely to hear from our patients and see what they have been up to.
Building the relationship
Over time I have built a good relationship with the University of Southampton and the academic podiatry team. The NK Active team host their students on clinical placement and supports the rehabilitation and clinical teaching on campus. In return, I hold a visiting lecturer status and receive mentorship from Professor Cathy Bowen. This has led to me being involved with wider research projects within the University.
Needing each other
From the early days of working with the University of Southampton, it became clear that both parties need each other. As clinicians we can be guilty of being fearful of research by not fully understanding the implications and what is involved. On the other hand, researchers need to know what the key questions are that should be investigated as well as see the variety of care services available to have a clear vision of how to implement evidence into clinical practice. It has been exciting going on this journey of blending education, research, and enterprise to try to benefit clinical practice.
Learning points
I do think that in healthcare we can be guilty of assuming that all research must be a double-blind randomised control trial (RCT) to be valid. However, an RCT may not be the correct methodology to help answer a question. Collecting your clinical data in the clinic is the start of a potential research journey.
I have found the use of data and regular audits helpful to assess what is working well, what needs improvement and where time should be wisely spent in my NKActive company. The audit data has also been useful to support my bids for work contracts.
Technology is your friend, with the rise and speed of technological advancements once you have set up your clinical data collection and audit process you can automate a lot of the data collection. You can also set up your electronic note templates to export the data that can be easily used for audit and research.
There will be errors along the way, and I made one in the early days which resulted in a large amount of my data not being useable.
It’s not just about the numbers, I started as someone who wanted to collect quantitative data but now, I look at my company and we have a pragmatic approach using both qualitative and quantitative data. I get the feel-good factor when I see the NK Active team and our patients succeed.
My final thoughts
Reflecting on my journey so far with implementing research into private practice, I am a strong advocate that we should all be doing this for the good of the profession. It’s not as scary as you think. I do not believe that being in private practice is a barrier, because as clinicians we have something to offer to the researchers and the researchers have something to offer to us. There are collaborations to be made, you just need to start by having the conversations.
My advice is to be open to change. Having an open mindset has been a strength that has allowed me to see the opportunities they have presented to me.
I have been very fortunate to have Charlie as part of our team and her role as a clinical academic has been invaluable in helping to build the bridges between clinical practice, research, and academia.
I am excited for the future to be involved in some larger projects and to start seeing some of our work published. Building working relationships, starting conversations and teamwork has positively impacted my company. As a podiatrist, running a private practice we have lots to offer.
Final thoughts from Nick:
‘Research is not as scary as you think. I do not believe that being in private practice is a barrier, because as clinicians we have something to offer to the researchers and the researchers have something to offer to us’
‘I have found the use of data and regular audits helpful to assess what is working well, what needs improvement and where time should be wisely spent in my company. The audit data has also been useful to support my bids for work contracts.’

Dr Paul Harradine PhD MSc BSc (Hons) CertEd
Independent podiatrist
Case study
Paul Harradine: independent podiatrist
My PhD career journey as a podiatrist in independent practice
‘My PhD has given me much more than the title’
I qualified in 1994 from the Northampton School of Podiatry. Looking back, my lecturers’ positive attitude towards continuing education and professional development influenced me greatly. Steve Avil was completing a diploma in Sports Medicine (a very rare thing for a podiatrist at that time) and Tim Kilmartin was finishing his fellowship and PhD. Both shared their enthusiasm openly with students, and I saw no reason why my degree was the end. If lecturers carried on researching and learning, then why wouldn’t we all?
Between 1994 and 2000 I obtained an MSc and a CertEd and spent a short three years lecturing undergraduate podiatry combined with an NHS clinical post. I worked long clinical hours (sometimes over 60 hours a week) combining full-time NHS with building a private practice, before becoming a full-time independent practitioner in 2005. From 2001 family life slowly took over, and I was blessed with five amazing sons over the next nine years.
I continued with small research projects and with theoretical peer review publications, squeezed in between family and clinical responsibilities. I lectured frequently on gait analysis and started to form a larger and more complex question: Was it possible to develop a real-time clinical gait analysis best practice approach to aid in the assessment of MSK lower limb injury? Was it possible to scale or score gait dysfunction, such as the FPI-6 is used for static foot posture?
Even with a background of publications and research, I failed. My attempts were rejected for publication. Looking back now, thank goodness they were. As well as being incomplete, my work was full of bias and assumptions. It would have been a step backwards for podiatry and evidence-based practice, not forwards.
With this frustration, I reached out to colleagues at the University of Southampton, and seven years ago I began my PhD. My initial experience with contacting my academic colleagues was completely positive, and I would advise any podiatrist interested in taking the research further to follow this approach. Ask those who know.
My PhD has changed me. Not just my professional life. The process is amazing, and my supervisors are some of the most patient, hardworking, and gifted professionals I have ever met. After completing my thesis, I was often asked “What would you do differently”. I’d answer “Nothing”. Although my work had many dead ends and difficulties, I needed to go through the development process of the PhD. It is hard, but if you trust the process and enjoy learning, it is incredibly fulfilling.
I’m not sure how much I will use the title “Dr” at work, as I’m aware it is confusing for patients. My family tries to ignore my “that’s what the Doctor ordered” one-liner every time Amazon deliver to our door. My PhD has given me much more than the title. I’ve added to the research in an area where there was hardly any. I’ve helped the podiatry profession move forward a little bit towards evidence-based practice and gait analysis. It has changed how I look at all research and every element of my practice. I believe I am a better clinician due to my PhD, and for that reason alone I would recommend anybody with an interest in research and a drive to improve to go for it!
Paul says:
‘I’ve added to the research in an area where there was hardly any, and I’ve helped the podiatry profession.
‘I believe I am a better clinician due to my PhD, and for that reason alone I would recommend anybody with an interest in research and a drive to improve to go for it!’

Louis Mamode
FCP portfolio case study
Case study
Louis Mamode: FCP portfolio case study
A limb/life-threatening presentation in primary demonstrating clinical excellence by a first contact podiatrist
A case of an undiagnosed DVT with a normal D-dimer result
Clinical presentation
Patient X was referred by his GP presenting with unilateral foot pain that had been present for 10 weeks. He presented with swelling and redness of the lower leg. The pain was located in the plantar metatarsal area and was worse on weight-bearing and palpation of his second and third metatarso-phalangeal joint (MTPJ) area. The patient did not report any trauma to this area and reports the pain gradually increases to the point where he is now unable to weight-bear for longer than an hour on his foot. Pain is not isolated to this area and can move proximally along the calf muscle. This is intermittent.
Previous assessments and tests
He had a recent D-dimer test which was normal.
Clinical tests and imaging
I suspected this still might be a DVT, I carried out the Wells' Score which was 3 with positive scores including calf swelling >3cm compared to contralateral side, unilateral leg swelling and unilateral pitted oedema.
I discussed this with my duty GP and arranged a duplex ultrasound which detected a femoral vein embolism, confirming the presence of a DVT. The patient was prescribed Rivaroxaban.
Differential diagnoses and your clinical reasoning
Differential diagnoses could include fractured metatarsal heads, capsulitis, and plantar plate tear which may have been suspected due to his location of foot pain. His X-ray also revealed lucency over the MTPJ area when compared to previous X-ray images taken 2 years earlier, osteopenia or osteoporosis, osteomyelitis or malignancy were possible differentials leading to loss of bone density, however this was only visible around the MTPJ and was not reported on the X-ray and may have been an artefact.
My clinical skills and history taking led me to believe the gentleman presented with atypical musculoskeletal symptoms and increased my suspicion of DVT despite a normal D-dimer result.
My reflection
I learnt that a normal D-dimer does not exclude the possibility of DVT and that strong celinical suspicion as well as a high Wells' Score warrants further investigation and referral to the vascular team.
This has impacted my practice as I will now incorporate the Wells' Score for any unilateral lower limb swelling and foot and ankle pain.
FCP portfolio case study
The management of a paediatric patient with metatarsalgia demonstrating clinical excellence by first contact podiatrist.
Case study
FCP portfolio case study
The management of a paediatric patient with metatarsalgia demonstrating clinical excellence by a first contact podiatrist
A case of Freiberg’s disease in a nine-year-old girl, early detection, and management
Previous history
A nine-year-old girl was booked into the out-of-hours first contact podiatry telephone consultation. This was done following a review with the GP who noted in the patient's record there was generalised pain in the second and third toe for several weeks, normal range of motion, no tenderness when assessed and examined, no clinical signs of infection and unable to find cause of pain and wanted a second opinion.
Following a telephone consult a face-to-face was offered the following day. Although I was not concerned about any red flags from our conversation, a physical assessment was deemed necessary.
Clinical assessment and presentation
Presentation of unresolved pain in the front of the foot and the patient had been walking on the side to avoid the painful area. The pain was unremitting, described as a dull ache and located only to the right foot with an impact on toe push off. The duration was three months with no history of trauma or injury. There was no hand pain noted, no sudden weight loss and no early morning stiffness reported.
Mum thought it was growing pains but was now concerned as it was affecting gait. The patient was in good health, systemically well and was engaging throughout the consultation. She reported no pain at night.
On assessment, there was bilateral syndactyly of the second and third toes. Examining the joints for a range of motion there was definite reduced dorsiflexion and plantarflexion of the second digit at the second metatarso-phalangeal joint (MTPJ) compared to the left foot.
Gait showed no abnormalities apart from reduced propulsion through the second metatarsal head to the right foot. Normal muscle strength and power were evident and unremarkable. There were no neurological concerns with 100% detection of 10g monofilament and normal reflexes. Pulses were palpable. There was no oedema and no erythema noted on the digits. The impact on life was that she was managing school, but PE was becoming difficult and the pain not improving.
Investigations
Based on the clinical findings I referred the patient for ultrasound and x-ray due to the reduced range of motion in the second metatarso-phalangeal joint.
Differential diagnoses and clinical reasoning
Differential diagnosis based on this presentation included fracture, Morton's neuroma, or Freiberg's. For me recognising what was a normal range of motion and what was acceptable was the most important aspect of the assessment and the type of pain that was being described. With the duration being three months, absent of trauma it was unlikely to be a fracture unless it was a stress fracture. Equally, both Morton's neuroma and Freiberg's can cause pain around this area.
The pain associated was not considered to be pins and needles nor was it a burning sensation - more like a dull ache, and no mention of a stone-like feeling on the ball of the foot nor like walking on a pebble.
Freiberg's was my initial preferred diagnosis, but I felt she may be too young. Though Love and O'Mara in 2010 reported it is found in all age groups from children to the elderly, Freiberg's most commonly affects adolescent females, with a 5:1 predominance over males. This is the only osteochondrosis that favours females more than males (Cerrato 2011). On examination, the patient demonstrated a reduced range of motion and pain around the second metatarsal head area, with no indication of injury and trauma so did have the feature of Freiberg's.
In referring for an X-ray this would rule out any fracture or any bony abnormality. If suspecting early Freiberg's, then an X-ray can often miss the features and the patient is often then misdiagnosed or discharged. Ultrasound can be much more effective at picking up earlier, subtle changes.
An ultrasound scan of the area was undertaken and an X-ray. The patient was fitted with an off-loading device and appropriate follow up arranged with a safety net in case of any issues.
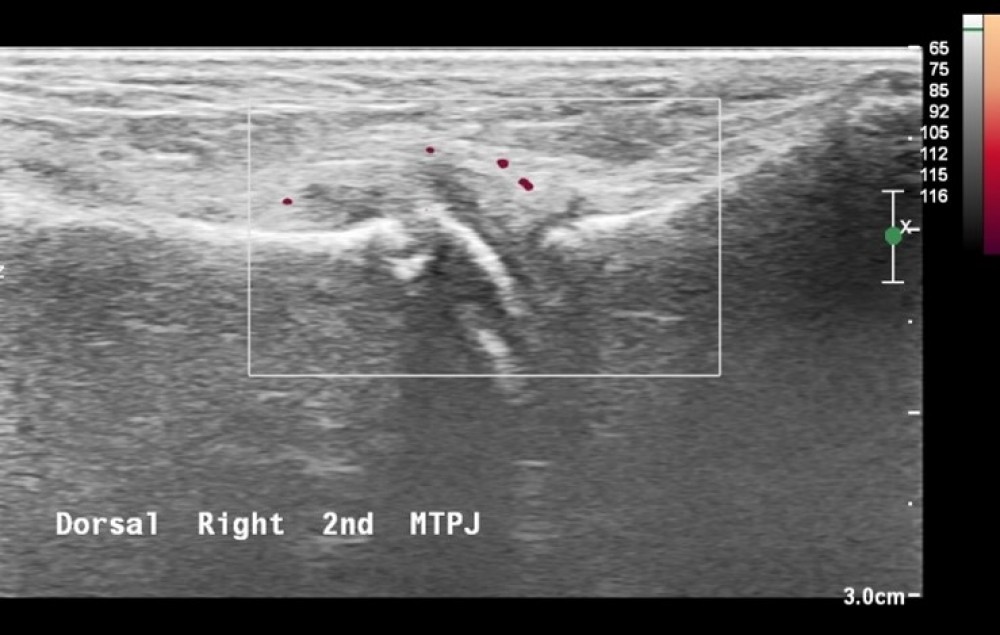
Image: Ultrasound of right forefoot showing increased vascularity to the dorsal second MTPJ, joint effusion and distension.
The ultrasound scan of the patient's foot shows joint effusion around the second MTPJ and a distended joint capsule. The report suggests some periosteal surface irregularity on the neck of the metatarsal – which could be deemed as age-related ossification, however, is relevant to the other pathology and the clinical symptoms.
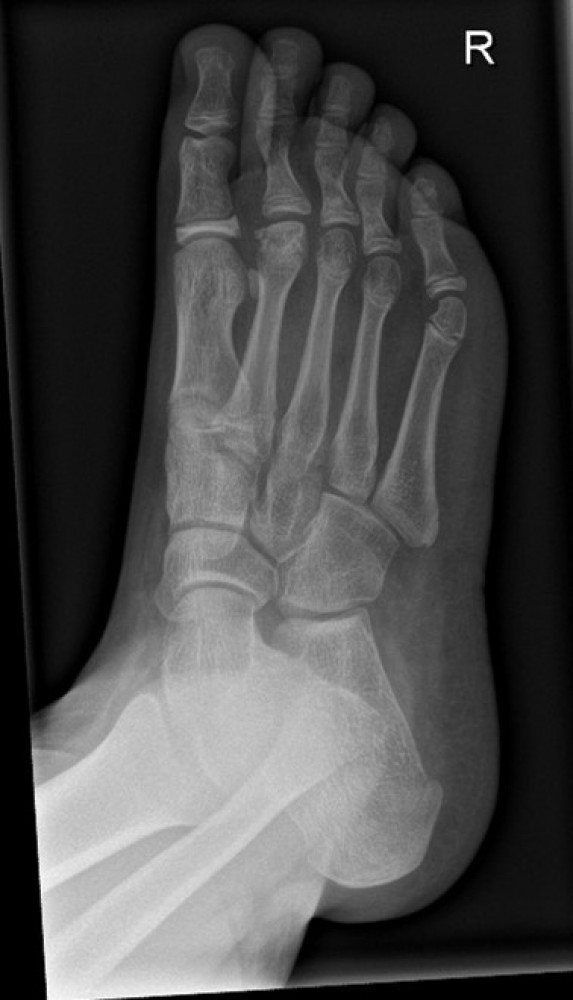
Image: X-ray shows Freiberg's disease with flattening of the second metatarsal head
Early detection
Early detection and treatment of this pathology are needed. This allows for the appropriate conservative treatment to be delivered to prevent needing surgery, reduce pain levels for the patient, and improve outcomes.
Presenting symptoms can be minimal with problems developing later in life if not managed appropriately. It can vary in severity and may develop over time. Complex cases can cause the bone to breakdown, causing early arthritis in the joint and leading to long-term problems, such as pain, unable to wear certain footwear, and participate in activities.
What is essential is early detection of this condition to allow for appropriate treatment options to prevent long-term effects on the foot.
Reference
Cerrato, R.A. (2011). Freiberg’s Disease. Foot and Ankle Clinics, 16(4), pp.647–658. doi:10.1016/j.fcl.2011.08.008.
Love, J.N. and O’Mara, S. (2010). Freiberg’s Disease in the Emergency Department. The Journal of Emergency Medicine, 38(4), pp.e23–e25. doi:10.1016/j.jemermed.2007.10.028.
FCP portfolio reflection
A case of spontaneous superficial thrombophlebitis and arterial occlusion
Case study
FCP portfolio reflection
A case of spontaneous superficial thrombophlebitis and arterial occlusion
In September 2021, a female patient aged 77 was triaged to my clinic with a history of left lower leg pain and redness over her superficial vein which was previously treated with antibiotics as cellulitis. Her main symptoms were:
- Burning sensation around the shin area near a varicose vein
- Pain keeping her up at night
- Both legs feel heavy when walking, doesn’t have to walk very far
- Her pain is worse first thing in the morning but improves with weight-bearing
- She recalls insect bites during an evening out but cannot be certain she was bitten on her leg
- She is not usually very active
- Does not smoke, is pre-diabetic and not on anti-hypertensive medication.
I treated her with one week of fluclox 500mg QDS due to possible infection but my main concern was the sign of intermittent claudication so I booked her for an ankle brachial pressure index (ABPI) test follow-up with me.
The patient was followed up by a GP one week after seeing me who prescribed further abx. A few days after her ABPI results were: R: 0.55 mmHg and L: 1.3 mmHg.
Her left pedal pulses were absent but her right pedal pulses were present. The right doppler was monophasic. This suggest to me the possibility of occlusion and I referred her to the vascular team.
In the meantime, the patient was experiencing further left shin redness and itching and was prescribed further antibiotics and steroid cream; her left toe was also red and swollen which was diagnosed as Gout and she was prescribed colchicine but the vascular surgeon believed this was related to her occlusion.
Exactly two months after her first symptoms she was seen by a vascular consultant who suspected underlying ischaemia, noted that her left foot looked quite a different colour to her right one in the supine position, and following a duplex scan highlighted occlusive disease in her arteries. She is now awaiting a CT scan for keyhole angioplasty.
Reflection
From her original presentation, this appeared more than an infected bite. The physical presentation of the patient’s leg suggested her problem was more vascular. There was low suspicion of DVT therefore I did not believe she had to be urgently referred to vascular. Through clinical reasoning, I referred her for an ABPI to investigate my suspicion/differential diagnosis.
The outcome led to the patient being seen by vascular within two months of presenting with symptoms of what appeared to be spontaneous superficial thrombophlebitis. From a review of the current literature, she could have potentially been treated with NSAIDs or low molecular weight heparin. However the ‘wait and see approach’ is also appropriate and would satisfy this case.
Impact on your practice: What will you do the same, or differently, next time, and why?
I could have perhaps provided continual care to the patient: she was prescribed several antibiotics whilst waiting for a vascular opinion for suspected cellulitis. However, I believe this was warranted as the redness and focal point were not directly on the varicose veins which was also confirmed by another practitioner.
Before seeing this patient, I was new to the general practice but aware of the referral pathway to the vascular team. Via a routine referral, it took two months for this patient to be seen leading to no improvement in her shin and a development of an ulcer on her left big toe. Since then I have visited the vascular team at the hospital and forged a direct link with the vascular podiatrist and nurses which will allow me to fast-track increasing or at-risk patients, or ask for specialist advice when needed, changing my future practice in vascular cases.
FCP case study
The management of a patient presenting with heel pain demonstrating clinical excellence by first contact podiatrist
Case study
FCP case study
The management of a patient presenting with heel pain demonstrating clinical excellence by first contact podiatrist
Previous history
The patient initially presented in my FCP Podiatry clinic reporting a new onset of heel pain after being triaged and signposted by the administrative team at his local GP practice.
The patient in this case study was a 35-year-old male with a medical history that includes psoriasis, hypertension and overweight with an eight-week duration of heel pain.
Clinical assessment and presentation
The pain was described to the right heel and indicated by the patient to involve the whole heel. The pain described as a dull ache most of the day and a sharp needle sensation in the heel for the first steps in the morning. Symptoms are relieved by cushioning under the heel and resting and are worse after rest, the first step in the morning and after a long day. Symptoms are also aggravated by walking barefoot. Verbal rating scales for pain were first steps of the morning 7/10 on VAS and during day 3/10.
Throughout the assessment lots of diagnoses were ruled out due to clinical features. Firstly, I was able to determine the likelihood of a red flag presentation was slim as the pain had a mechanical pattern to it as most red flag pains tend to hurt in a pattern different to this (NHS, 2021). There was no night pain or sudden weight loss reported on questioning for example.
The patient's symptoms are classical to plantar fasciopathy given the post-static dyskinesia symptoms. Post- static dyskinesia pain in the heel is largely associated with ligament and tendon complaints of a mechanical origin and these can then be differentiated based on location of pain. (Alshami, Souvlis & Coppieters, 2008)
Diagnosis and clinical opinion
The following differential diagnoses were considered: heel fat pad atrophy, calcaneal stress fracture, and insertional Achilles tendonitis. They were also ruled out as unlikely due to the location of the heel pain and its classical presentation with waxing and waning features.
The diagnosis was explained to the patient. I tend to explain plantar fasciopathy from a stress and strain standpoint (Korhonen & Saarakkala, 2011). It is my experience that patients tend to feel that non-medical treatments have a greater benefit when the rationale behind them is explained. By detailing to a patient the concept of stress vs strain we can now explain the difference between plantar fasciitis and plantar fasciopathy. This explanation I feel also drives home the importance of relative rest as a required treatment.
Over 95% of patients within my caseload presenting with this plantar fasciopathy symptoms will be sent away from the first consultation with the following treatments:
- Stretching
- Strengthening
- Advice on footwear (and wearing footwear at home)
- Advice on orthoses if they are assessed using physical assessment as suited to this
- Taping.
When we consider patients might forget between 40%-80% of what is said in a consultation (Kessels, 2003) I also always follow up with:
- A text message containing a patient information leaflet on plantar fasciopathy
- Exercises sent via physiotherapy-centred video software
- A text telling the patient if they are not feeling better or seeing some improvement by 12 weeks then they should return to my care.
Follow-up and investigations
In this patient’s case, I revisited the idea of a possible systemic inflammatory cause. An ultrasound scan was agreed upon as it would help rule out other possible diagnoses such as heel bursitis and help toward confirming the diagnosis of plantar fasciopathy by demonstrating thickening of the fascia itself. If the ultrasound returned suggesting a florid swelling response (likely commented as hypoechogenicity on the US report), or lots of extra-articular features such as calcification at the Achilles tendon insertion, then the possibility of a systemic cause is once again reconsidered (Ieong, Afolayan, Carne & Solan, 2013).
In the meantime, the patient was asked to keep up with his conservative care of stretching, strengthening, footwear changes and taping. I also advised a bit further at this consultation on the value of insoles and signposted toward a particular device the patient might find helpful.
Follow-up appointment after imaging 7 weeks later
In this patient’s case, the ultrasound results suggested thickening of the medial fascia band with minimal other changes noted. I now discussed the options with the patient: his options, in this case, were either a steroid injection or a consideration of whether or if he would like to privately fund a course of shockwave therapy. We discussed the risks and benefits of each of these treatments and the pros and cons, considering one of the treatments had a financial attachment (Morrissey et al, 2021)
The patient opted at this juncture to have a steroid injection so appropriate literature was provided and an injection was booked for two weeks later.
Injection appointment
A landmark injection was provided into the right heel with a depomedrong and lidocaine mixture.
The follow-up phone call two weeks later
The patient reported a complete resolution in his heel pain at two weeks post injection. The patient reported no side effects from the injection.
Follow-up at 18 weeks
A follow-up call was completed at 18 weeks simply for the reason of completing this case study to assess if the patient's heel pain had remained resolved. The patient reported no return of symptoms.
Summary
This patient was consulted a total of five times during his management and two of these appointments were planned reviews. Assessment and management included considerations around requesting bloods, requesting appropriate diagnostic imaging and considering if onward referrals were required. Outside of the imaging the rest of the patient’s care was directed by one clinician: the FCP Podiatrist. The patient did not consult another member of the primary care during his period of care.
This case study demonstrates effective triage into the FCP Podiatrist clinic, effective safety netting and red flag screening, effective diagnostic and treatment skills and a good outcome for a patient without the need for onward referral or involvement of medical colleagues who were therefore freed up to treat other patients. The patient was under my care for 30 weeks.